New Research Reveals How IBD Creates Lasting Changes That May Increase Cancer Risk
Summary of Unknown
IBD Movement provides news analysis and insights for the IBD community. Always consult your healthcare provider for personal medical advice.
Understanding the Long-Term Impact on Your Colon Health
If you’re living with inflammatory bowel disease, you’ve likely heard about the increased risk of colorectal cancer that comes with chronic inflammation. But groundbreaking new research is shedding light on exactly how this happens at the cellular level – and why the effects of inflammation may persist long after your symptoms have quieted down. This discovery could fundamentally change how we think about IBD management and long-term health monitoring, offering both important insights and new hope for prevention strategies.
For many in our community, the relationship between chronic inflammation and cancer risk has been a source of ongoing concern. This research helps us understand the biological mechanisms at work, which is the first step toward developing better ways to protect ourselves and potentially interrupt these harmful processes.
What the Research Discovered
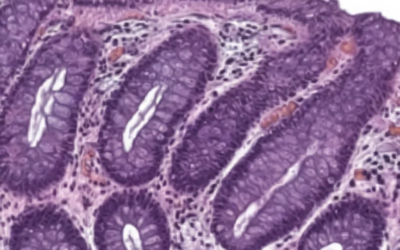
According to the research published in News Medical, scientists have made a significant breakthrough in understanding how chronic colitis affects colon stem cells at the most fundamental level. The study revealed that chronic inflammation doesn’t just cause temporary damage – it actually creates a lasting “epigenetic memory” in the stem cells that line our colons.
The researchers found that this cellular memory persists for more than 100 days after recovery in their mouse models, which is particularly striking given that mice have much shorter lifespans than humans. This suggests the effects could last much longer in people with IBD. The memory is characterized by specific changes in chromatin – the complex of DNA and proteins in our cells – that are linked to a cellular pathway called AP-1.
Most concerning was the discovery that these persistent changes later amplify tumor growth when oncogenic (cancer-causing) mutations occur. In essence, the inflammation from colitis appears to prime colon stem cells in ways that make them more susceptible to becoming cancerous later, even after the original inflammation has resolved.
What This Means for People Living with IBD
This research provides crucial insights into why people with IBD face an elevated risk of colorectal cancer, but it also opens up new avenues for understanding and potentially preventing this complication. The concept of “epigenetic memory” helps explain why cancer risk remains elevated even during periods of remission – something many of us have wondered about.
For those of us managing Crohn’s disease or ulcerative colitis, this finding underscores the critical importance of achieving and maintaining deep, sustained remission. It’s not just about feeling better day-to-day; it’s about preventing these long-term cellular changes that could have serious consequences years down the road. This research suggests that every flare, every period of active inflammation, may be leaving a lasting mark on our colon stem cells.
The study also highlights why early intervention and aggressive treatment of IBD may be so important. If chronic inflammation creates these persistent changes, then preventing or minimizing inflammation from the very beginning of the disease course could be key to reducing long-term cancer risk. This supports the growing trend toward “treat-to-target” approaches in IBD care, where the goal isn’t just symptom relief but objective measures of healing.
However, it’s important to note that this research was conducted in mice, and while mouse models of colitis share many similarities with human IBD, we can’t directly translate these findings to humans without further study. The timeline of 100+ days in mice would likely correspond to a much longer period in humans, but we don’t yet know exactly how long these epigenetic changes persist in people with IBD.
This discovery also raises important questions about surveillance and prevention strategies. Currently, people with IBD undergo regular colonoscopy screening for colorectal cancer, typically starting 8-10 years after diagnosis. Understanding that inflammation creates lasting cellular changes might influence how we think about the timing and frequency of this screening.
The research could also pave the way for new therapeutic approaches. If scientists can understand exactly how these epigenetic changes occur and persist, they might be able to develop treatments that could reverse or prevent them. This could include medications that target the specific AP-1 pathway mentioned in the study, or therapies designed to “reset” the epigenetic memory in colon stem cells.
For many in our community, this research may also provide validation for the fatigue and long-term effects we experience. Even when our IBD appears to be in remission, our bodies are still dealing with the cellular consequences of past inflammation. This biological evidence supports what many of us have long suspected – that IBD has lasting effects that extend beyond active symptoms.
Expert Context and Clinical Implications
Gastroenterologists and IBD specialists have long observed the connection between chronic inflammation and increased cancer risk, but this research provides new molecular-level understanding of the mechanisms involved. The concept of epigenetic memory in stem cells represents a significant advancement in our understanding of how inflammatory diseases contribute to cancer development.
This type of research is particularly valuable because it suggests that the window for prevention may be longer than previously thought, but also that the effects of inflammation may be more persistent. Patients should discuss with their healthcare providers what this means for their individual monitoring and treatment plans, especially if they have a history of poorly controlled inflammation or multiple flares.
The findings also support the importance of comprehensive IBD management that goes beyond just treating symptoms to focus on achieving mucosal healing and preventing long-term complications.
Actionable Takeaways for IBD Patients
- Prioritize sustained remission: Work closely with your healthcare team to achieve and maintain the deepest level of remission possible, as this research suggests every period of active inflammation may have lasting effects.
- Stay current with screening: Continue following your doctor’s recommendations for colorectal cancer screening, and discuss whether your personal history of inflammation should influence your screening schedule.
- Focus on inflammation reduction: Consider lifestyle factors that may help reduce inflammation, including stress management, adequate sleep, and following your prescribed treatment regimen consistently.
- Ask about monitoring options: Discuss with your doctor whether additional monitoring tools, such as fecal calprotectin or other inflammatory markers, might help track your inflammation levels more precisely.
- Stay informed about emerging treatments: As research like this advances, new therapeutic options targeting these cellular pathways may become available.
Looking Forward with Hope and Knowledge
While this research reveals concerning aspects of how IBD affects our bodies at the cellular level, it also represents tremendous progress in understanding the disease. Knowledge is power, and the more we understand about how IBD works, the better equipped we become to fight it effectively.
This discovery opens up new research directions that could lead to breakthrough treatments specifically designed to prevent or reverse the epigenetic changes caused by chronic inflammation. It also reinforces the importance of the comprehensive, proactive approach to IBD care that many of us are already pursuing.
As always, we encourage our community members to discuss these findings with their healthcare providers and to continue advocating for the best possible care. Together, we can use this new understanding to work toward better outcomes and a future where the long-term consequences of IBD are preventable.
Source: This post summarizes reporting from Unknown. Read the original article.