Breakthrough Research Reveals How Mucosal Glycans May Hold the Key to IBD Treatment
Summary of BIOENGINEER.ORG
IBD Movement provides news analysis and insights for the IBD community. Always consult your healthcare provider for personal medical advice.
If you’re living with inflammatory bowel disease (IBD), you’ve likely wondered why your immune system seems to attack your own digestive tract. New research into mucosal glycans—complex sugar molecules that line our intestines—is providing fascinating insights that could revolutionize how we understand and treat conditions like Crohn’s disease and ulcerative colitis. This emerging field of study suggests that these microscopic guardians of our gut may play a far more crucial role in IBD development and progression than previously understood, offering hope for more targeted and effective treatments in the future.
What the Research Reveals
According to BIOENGINEER.ORG, recent scientific investigations have identified mucosal glycans as key players in the development and progression of inflammatory bowel disease. These complex carbohydrate structures, which form a protective barrier along the intestinal wall, appear to be significantly altered in people with IBD compared to healthy individuals.
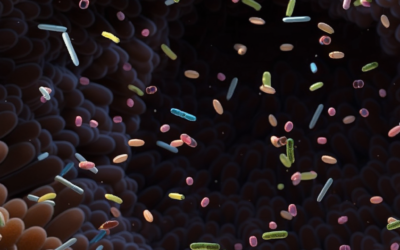
The research highlights how these glycan molecules serve as critical mediators between the gut microbiome and the immune system. When functioning properly, they help maintain the delicate balance that prevents harmful bacteria from penetrating the intestinal barrier while allowing beneficial microorganisms to thrive. However, in IBD patients, these protective molecules show distinct structural and functional changes that may contribute to the chronic inflammation characteristic of these conditions.
Scientists have discovered that the composition and arrangement of mucosal glycans differ markedly between healthy individuals and those with Crohn’s disease or ulcerative colitis. These differences appear to affect how the immune system responds to intestinal bacteria, potentially triggering the inappropriate inflammatory responses that define IBD.
The study also suggests that understanding these glycan alterations could lead to new diagnostic tools and therapeutic approaches, representing a significant shift from current treatment strategies that primarily focus on suppressing immune system activity.
What This Means for the IBD Community
This research represents a paradigm shift in how we understand IBD at the molecular level, and the implications for patients could be profound. For years, the IBD community has known that the condition involves a complex interplay between genetics, environment, immune function, and gut bacteria. Now, mucosal glycans appear to be the missing piece that helps explain how these factors work together to trigger and sustain chronic inflammation.
For people living with IBD, this discovery offers several reasons for cautious optimism. First, it provides a clearer picture of why current treatments work for some patients but not others. If mucosal glycan patterns vary between individuals, it could explain why medications like biologics show such variable response rates. Understanding these differences might eventually allow doctors to predict which treatments are most likely to work for specific patients, moving us closer to truly personalized medicine.
The research also opens up entirely new avenues for treatment development. Instead of broadly suppressing the immune system—which is how many current IBD medications work—future therapies might target the specific glycan abnormalities that contribute to inflammation. This could potentially lead to treatments that are both more effective and have fewer side effects, addressing one of the biggest challenges in current IBD management.
Perhaps most intriguingly, this research suggests that dietary interventions might play a more significant role in IBD management than previously thought. Since glycans are carbohydrate-based molecules, and our diet directly influences the types of bacteria in our gut, there may be ways to support healthy glycan function through targeted nutritional approaches. This doesn’t mean that diet alone can cure IBD, but it reinforces the importance of working with healthcare providers to optimize nutrition as part of comprehensive treatment plans.
The discovery also has implications for understanding IBD flares and remission periods. If glycan function fluctuates over time, it might help explain why symptoms can be unpredictable and why some patients experience periods of stability followed by sudden flare-ups. This understanding could eventually lead to better monitoring tools that help predict and prevent flares before they occur.
For patients who have struggled with treatment-resistant IBD, this research offers hope that new therapeutic targets are on the horizon. The complexity of glycan biology means there are multiple potential intervention points, increasing the likelihood that effective treatments can be developed even for the most challenging cases.
However, it’s important to maintain realistic expectations about timeline. While this research is exciting, translating these discoveries into practical treatments typically takes years of additional research, clinical trials, and regulatory approval. The IBD community has learned to balance hope with patience when it comes to promising research developments.
Expert Perspective on Clinical Implications
Gastroenterologists and IBD specialists are increasingly recognizing that the intestinal barrier function extends far beyond simple physical protection. The glycan layer represents a sophisticated biological interface that requires careful maintenance for optimal health. Experts suggest that patients should discuss with their healthcare providers how this emerging understanding might influence their current treatment approach.
Medical professionals emphasize that while this research is promising, it’s still in relatively early stages. Patients should continue following their established treatment plans while staying informed about developments in glycan research. The complexity of these molecules means that therapeutic applications will require extensive testing to ensure both safety and efficacy.
Healthcare providers also note that this research reinforces the importance of comprehensive IBD management, including attention to gut microbiome health, stress management, and nutritional optimization—all factors that may influence glycan function.
Actionable Takeaways for IBD Patients
- Stay informed but patient: While this research is exciting, practical applications are likely years away. Continue current treatments while monitoring developments in glycan research.
- Discuss microbiome health with your doctor: Since glycans interact closely with gut bacteria, optimizing microbiome health through probiotics, prebiotics, or dietary changes may be beneficial.
- Consider participating in research: If opportunities arise to participate in studies related to glycan function or microbiome research, discuss the potential benefits and risks with your healthcare team.
- Maintain comprehensive care: This research reinforces the importance of addressing all aspects of IBD management, including nutrition, stress, sleep, and medication adherence.
- Ask about personalized medicine approaches: Inquire whether your healthcare provider uses or plans to incorporate biomarker testing that might eventually include glycan analysis.
Looking Forward with Hope and Realism
The discovery of mucosal glycans as key players in IBD represents one of those moments when scientific understanding takes a significant leap forward. For a community that has long awaited breakthroughs in treatment options, this research offers genuine reason for optimism about the future of IBD care.
While we await the translation of this research into practical treatments, the IBD community can take comfort in knowing that scientists are uncovering the fundamental mechanisms that drive these conditions. Each new discovery brings us closer to more effective, targeted therapies with fewer side effects.
What questions does this research raise for you about your own IBD journey? Share your thoughts and experiences in the comments below—your insights help strengthen our community’s understanding and support network as we navigate these exciting developments together.
Source: This post summarizes reporting from BIOENGINEER.ORG. Read the original article.